Designated Diagnostic Providers
Using your benefits for outpatient lab and major imaging services

Maybe you've heard about Designated Diagnostic Provider benefits or maybe it's a new benefit to you. If you get your health insurance through your employer, it's important to know the details because it may affect your coverage for outpatient lab and major imaging services. Major imaging services are CTs, MRA/MRIs, PET and nuclear medicine scans. Let's go over what it is and how it works.
What is a Designated Diagnostic Provider?
Designated Diagnostic Providers are laboratory providers and imaging centers that meet certain quality and efficiency requirements. If you have a Designated Diagnostic Provider benefit, you’ll have the highest level of coverage — and likely save money — when you use Designated Diagnostic Providers for your outpatient lab and/or major imaging services.
How do I know if I have Designated Diagnostic Provider benefits?
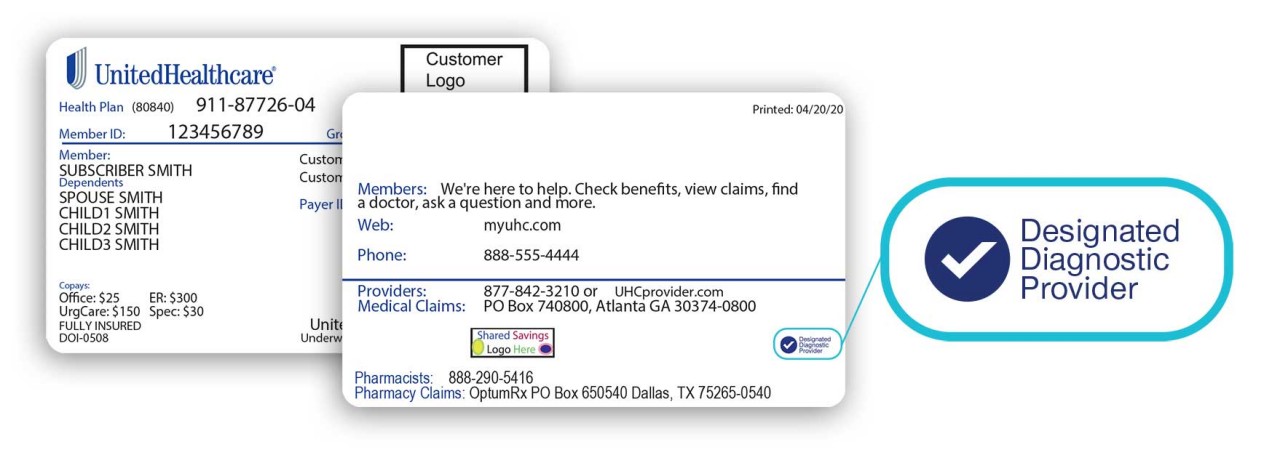
Designated Diagnostic Provider benefits are included with specific plan types. If you have these benefits, you should have received a new health plan ID card that shows that you have Designated Diagnostic Provider benefits.
Sign in to learn if Designated Diagnostic Provider benefits apply to your health plan. If you have Designated Diagnostic Provider benefits and you don’t use a Designated Diagnostic Provider, you may have a higher cost-share and end up paying more out-of-pocket for your outpatient lab and/or major imaging services.
How do I find a Designated Diagnostic Provider?
To find a Designated Diagnostic Provider near you, sign in to myuhc.com and select Find Care and Costs or use the UnitedHealthcare app. Look for the green check that indicates a provider is a Designated Diagnostic Provider. Here's an example:

When do I need to use a Designated Diagnostic Provider for lab tests or major imaging services?
Using a Designated Diagnostic Provider may help you save money on many common lab and/or major imaging services. If you need lab or major imaging services, be sure to tell your doctor which Designated Diagnostic Provider to use. Designated Diagnostic Provider benefits apply to most outpatient services, including:
Frequently asked questions (FAQs) about Designated Diagnostic Providers
Designated Diagnostic Provider benefits help protect members from higher, unjustified costs for outpatient lab or major imaging services while maintaining access to quality, safe, and efficient providers. These benefits are part of a strategy to lower overall healthcare costs.
Member benefits for outpatient diagnostic lab and major imaging services will be maximized when using Designated Diagnostic Providers that meet certain quality and efficiency requirements. If outpatient lab or major imaging services are performed by a non-Designated Diagnostic Provider, you may have a higher cost-share and end up paying more out-of-pocket for those services.
We created Designated Diagnostic Provider benefits to focus on outpatient lab and major imaging service providers that drive the best quality and efficiencies to deliver a better experience, better health outcomes, and lower costs.
The following are services that do not apply for Designated Diagnostic Provider benefits:
- Outpatient surgery pre-operation testing that is billed as part of a global surgical package
- Services billed as a component of a bundled charge
- Services billed as part of an ER service, with same date of service
- Services billed as part of an outpatient surgery event, with same date of service
- Services billed as part of pre-admission testing, with same date of service
- Services billed as part of an inpatient event, with same date of service
- Services billed as part of an observation event, with same date of service
- Lab procedures billed as part of an Infertility treatment
Lab and major imaging services do not apply when performed as part of:
Designated Diagnostic Provider Imaging cost shares do not apply to children under the age of 7.
Designated Diagnostic Imaging is for major imaging only (CT, MRI/A, PET and Nuclear); it does not apply to imaging such as ultrasound, mammogram, and x-ray.
Designated Diagnostic Provider benefits apply to any outpatient lab or major imaging service performed in a free-standing or outpatient hospital lab or imaging setting. Any labs or major imaging services performed in your doctor’s office will be covered as in-network per your plan benefits.
Designated Diagnostic Provider benefits only apply to outpatient diagnostic lab or major imaging services.
Visit myuhc.com, or use the UnitedHealthcare Mobile app on your smartphone. Select Find a Doctor to search for providers near you. Designated Diagnostic Providers will be identified in search results with a green check mark. You can also call the member phone number on your health plan ID card.
For members who may not have access to Designated Diagnostic Providers because of their geographic location, UnitedHealthcare will look into each situation and work with the nearest hospitals, labs, imaging centers, or clinics to ensure they meet quality and efficiency requirements to serve as a Designated Diagnostic Provider. If you can’t find a Designated Diagnostic Provider, contact us by calling the number on your health plan ID card.
UnitedHealthcare has invited all in-network free-standing labs and outpatient hospital labs and major imaging facilities that meet the quality and efficiency criteria to become a Designated Diagnostic Provider.
Designated Diagnostic Providers are in-network providers who have achieved additional designation based on quality and efficiency standards. Non-Designated Diagnostic Providers are still considered in-network providers, however, services received from a non-Designated Diagnostic Provider are covered at a lower benefit level when compared to a Designated Diagnostic Provider. Designated Diagnostic Providers are never out-of-network providers.
Talk to your doctor about the need to use a Designated Diagnostic Provider for your outpatient lab and/or major imaging services. We are working with all doctors to ensure referrals are made to Designated Diagnostic Providers, but you can help by making sure your doctor understands that your lab or major imaging work should be done at or sent to a Designated Diagnostic Provider. Your online search tool and the one used by your doctor both clearly indicate labs or major imaging services that are designated.
Ask your provider if the location that you have been referred to is considered a Designated Diagnostic Provider. Your doctor should refer you to a Designated Diagnostic Provider to ensure you have the best coverage and lowest price under your UnitedHealthcare plan.
If your doctor’s office is a Designated Diagnostic Provider, there will be no change to your lab or major imaging care routine. If they are not a Designated Diagnostic Provider, you should speak to your doctor about switching or sending your lab or major imaging work to a Designated Diagnostic Provider.
If the specialty facility is a non-Designated Diagnostic Provider, your doctor can call the UnitedHealthcare provider services call center to get more information about appropriate coverage.
If you have lab or major imaging services that were done at a non-Designated Diagnostic Provider, you may have a higher cost-share and end up paying more out-of-pocket for those services. For the highest level of coverage, make sure your lab and major imaging services are done at a Designated Diagnostic Provider.
You can contact us with questions by calling the member phone number on your health plan ID card.
Looking for other ways to save money on health care?
Explore more ways to control your costs and make health care more affordable for all.