What you need to know about mammograms and breast cancer screening
Breast cancer is the second most common cancer in women — and in 2023, an estimated 280,000 women were newly diagnosed.
These statistics, in combination with new research, has led to a proposal by the U.S. Preventive Services Task Force to recommend breast cancer screening every other year, beginning at age 40 and continuing until age 74. This is a shift from the previous recommendation that women begin screening at age 50 every two years or begin screening at age 40, based on individual preference and need.
One in eight women in the U.S. has a chance of developing breast cancer, but it is also highly treatable with early detection. According to the American Cancer Society, regular screening tests or mammograms are the most effective way to detect any abnormalities that may indicate cancer.
The Task Force states part of its recommendation is to help eliminate health disparities that can exist, particularly for Black women who are 40% more likely to die from breast cancer and often receive cancer diagnoses earlier in life.
2D mammogram vs. 3D mammogram
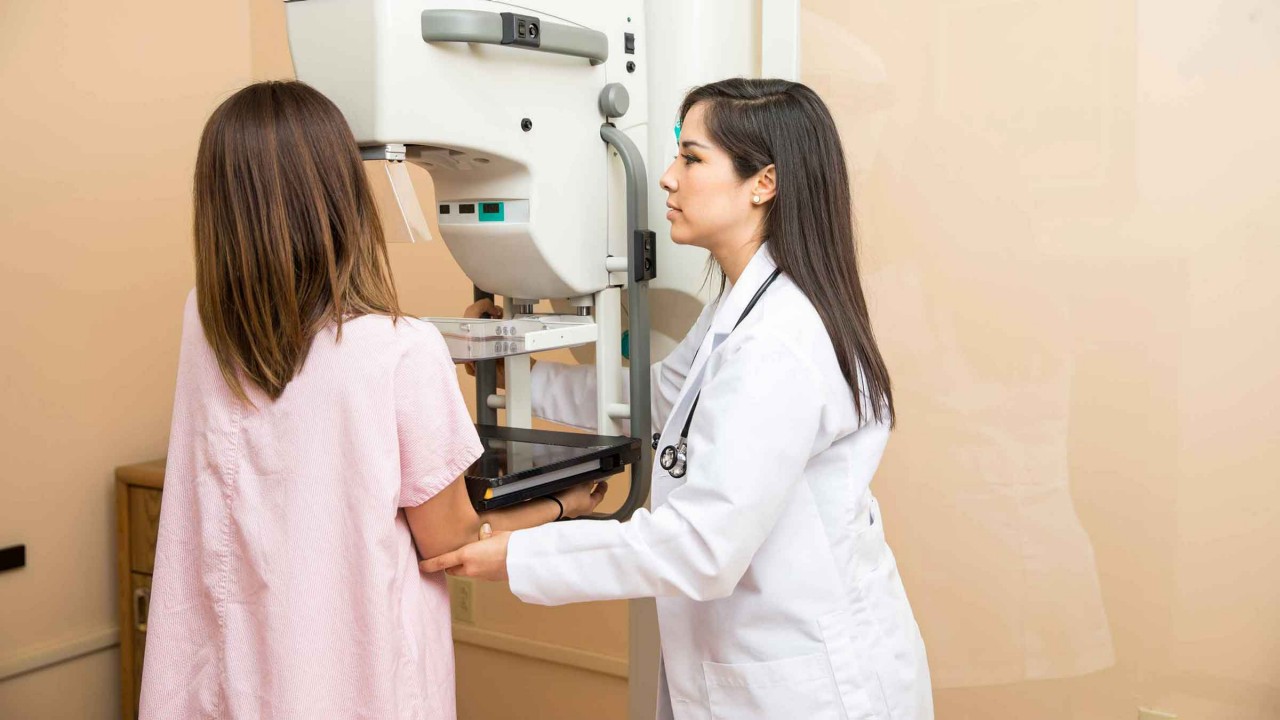
For many years, the only mammogram option was a two-dimensional version. During this type of procedure, a picture is taken of the entire breast in two directions: from top-to-bottom and side-to-side.
The 2D mammogram is the recommended standard in breast cancer screenings, but there is research showing about half of women getting annual 2D screenings over a 10-year period may have a false-positive finding at some point.
When the breast gets compressed, it can cause the tissue to overlap, possibly reducing the reliability of the test to detect cancer. For women with dense breast tissue — typically half of women who receive mammograms — detection can be difficult and may require additional screening tests.
Advanced screening options use three-dimensional technology to create a clearer image. Research suggests breast tomosynthesis, also known as 3D mammography, may reduce the need for follow-up imaging and improve breast cancer detection, especially with dense breast tissue.
Both are effective in screening for breast cancer.
Clinical and self-screening
In addition to imaging to screen for breast cancer, clinical examinations and self-exams can be helpful in identifying any changes or new issues.
A clinical exam is performed by a doctor to check for any abnormalities, lumps or other warning signs. A breast self-exam can be done once a month to help you regularly know your body and when things may feel different or new lumps appear.
Every year, an estimated 300,000 women are diagnosed with breast cancer in the U.S. Learning more about the best method for mammography could help you feel more informed to have a conversation with your health care provider on what might be best for you.
Coverage for different screening tests will depend on your individual health plan.