When you’re eligible to delay enrollment in Medicare because you have creditable employer coverage (through your employer or a spouse’s employer) you qualify for an 8-month Special Enrollment Period (SEP). During this time, you’ll be able to enroll in Medicare.
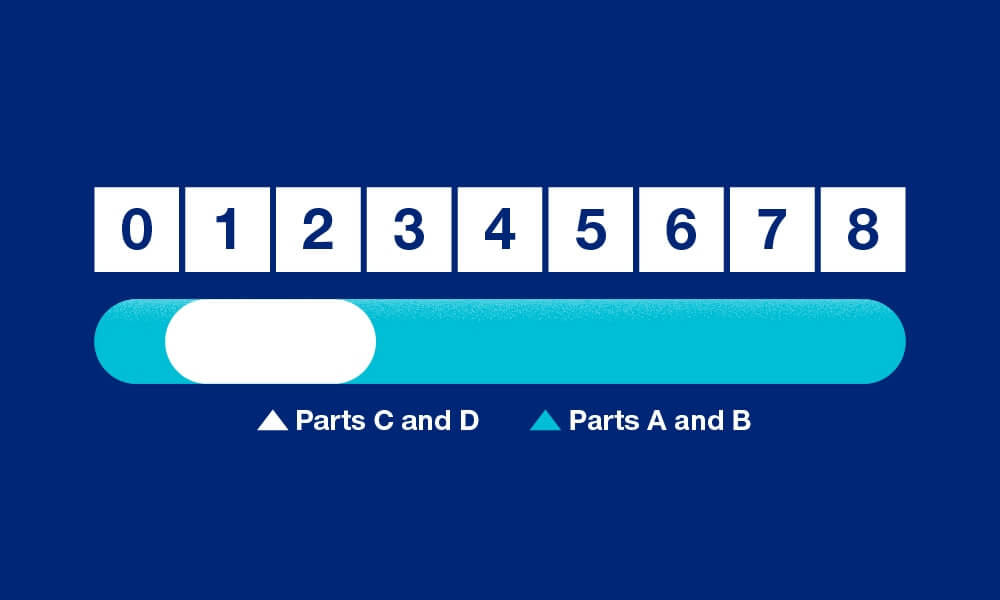
Your Special Enrollment Period begins when you retire or lose your employer coverage, whichever happens first. You will have up to 8 months to enroll in Parts A and/or B, but only the first two months to enroll in Parts C and/or D.
How to use your Special Enrollment Period
When you’re ready to enroll in Medicare, you will have a full 8 months to enroll in Parts A and/or B but only the first two months of this period to enroll in Parts C and/or D. Watch the video below to help you understand how to enroll during your Special Enrollment Period after you lose employer coverage or stop working.
When to enroll in Medicare if you worked past 65

During your Special Enrollment Period, you have 8 months to enroll in Part B, and Part A, if you haven’t already, and you will have 2 months to enroll in a Medicare Advantage (Part C) or a Part D prescription drug plan.

An important note about Part D: You have exactly 63 days to get a stand-alone Part D prescription drug plan or a Medicare Advantage plan with prescription drug coverage included without penalty. After this time, you may be subject to the Part D late enrollment penalty which generally lasts as long as you have Medicare prescription drug coverage.
Finally, it is important to know that you are not eligible for this Special Enrollment Period when your COBRA or retiree coverage ends. However, you may be eligible for a different Special Enrollment Period specific to a qualifying life event.
About Medicare Made Clear
Medicare Made Clear brought to you by UnitedHealthcare provides Medicare education so you can make informed decisions about your health and Medicare coverage.
Get the latest
Boost your Medicare know-how with the reliable, up-to-date news and information delivered to your inbox every month.
*All fields required

