The untold story: Controlling costs through payment integrity
Payment integrity solutions combat provider charge issues and optimize claim-payment processing to reduce expenses.
Of the $3.6 trillion spent on health care annually, the National Health Care Anti-Fraud Association estimates that tens of billions of dollars are lost due to health care fraud.1 The scale of this problem demands that insurers take responsive action and implement strategic solutions to avoid potentially serious financial losses for health plans.
There are many opportunities for errors, fraud and abuse in today’s increasingly tech-driven health care industry. Those seeking to profit from questionable claims also have easier access to tools and information that create business risk and increase possibilities for cost inefficiency.
UnitedHealthcare is working to drive greater savings and improved accuracy through solutions for payment integrity. It’s defined as the process of ensuring a health claim is paid:
- By the responsible party for eligible members
- According to contractual terms and policy
- Not in duplicate or error
- Free of fraud and abuse
These comprehensive programs are designed to identify and take action on invalid or inaccurate claims. Payment integrity is more than just a behind-the-scenes operational capability to help employers make sure their health plan is paying claims appropriately. Increasingly, it’s a strategic imperative for an industry looking to make health care more affordable for everyone.
“The thing about payment integrity is that it often goes unnoticed and therefore may be undervalued,” says Ruby Kam, Chief Financial Officer, National Accounts with UnitedHealthcare. “It’s important to remember that these programs are working, and they’re working well. They’re actively generating significant savings for our clients.”
3 key takeaways on health care fraud and abuse
- An effective payment integrity program uses everything from complex, automated technologies to focused, hands-on reviews by specialty physicians and claims professionals.
- Payment integrity approaches can vary widely among insurers, and the success or failure of these programs can significantly impact costs.
- One of the keys to effective payment integrity is getting in front of potential issues before a claim is paid, as this is the least disruptive time to provide accurate payment.
Payment integrity programs and technology
Many employers take for granted that health care dollars will be paid out only for fairly priced, necessary and eligible services used by eligible members. Given the nature of payment fraud and abuse, employers look to their insurers to help combat these wasted costs.
The insurer employs a highly advanced and coordinated system of controls to ensure claims are paid appropriately. This includes methods to prevent duplicate payments and payments for items or services not actually provided.
An effective payment integrity program is crucial during 3 key stages of claims processing:
- Pre-adjudication when eligibility of charges is established. This is the time to correct mistakes, assist with preauthorizations and prevent incorrect claims from entering the system.
- Prepayment when the claim has been received but not yet paid. This is the time to verify eligibility and ensure accurate payment.
- Recovery after the claim has been paid, but a refund is owed. Retrospective efforts ensure correct payment was made, incorrect payments are adjusted and issues are resolved in a timely manner.
“When we typically talk about ‘overpayments’ as part of recovery, a lot of people assume we made mistakes and then had to retrospectively recover the overpaid amount,” says Mike Laubsted, Vice President Payment Integrity Operations at UnitedHealthcare. “In fact, a large proportion of recoveries are made because our data mining has subsequently uncovered new information that wasn’t available when the original claim was paid and that new data is what allows us to make a better payment decision.”
The challenge is that the payment integrity approaches of various insurers can vary widely, and the success or failure of these programs can impact costs in significant ways. An effective payment integrity program is multi-faceted and includes, but is not limited to:
- Health care artificial intelligence
- Patterning algorithms
- Geographic price comparisons
- Machine learning
Proactive payment integrity
One of the keys to effective payment integrity is getting in front of potential issues before a claim is paid, as this is the least disruptive time to provide accurate payment. For example, coordination of benefit reviews can occur before the payment cycle begins, as can detailed reviews of payment policies that may affect the claim. UnitedHealthcare delivers for clients a $9.17 per member per month (PMPM) savings before a claim is paid.2
Before a claim even processes, reimbursement and reduction policies have been put in place to identify or flag potential issues, and adjust claims as necessary. UnitedHealthcare has over 60 reimbursement policies, with hundreds of edits within each policy. Three examples of these reimbursement policies are:
- Maximum Daily Frequency:This rule enforces guidelines for the maximum number of times a procedure or service can be billed each day.
- Example: An immunization can only be billed once per day. An appendectomy is limited to 1 procedure because a person only has 1 appendix.
- Technical Validation: This rule ensures accurate payment by preventing 2 entities from billing for the same technical component of a service.
- Example: An MRI, the technical component of the service, cannot be billed by both the facility and the physician who reads the results.
- Bundling: This rule ensures that multiple procedure codes are not billed for a group of procedures that should be covered by 1 comprehensive code.
- Example: Provider billed for screening and office visit separately when the screening would be included in the office visit.
Payment integrity capabilities like these have helped UnitedHealthcare deliver its clients a $34.86 PMPM total average savings through the entire process, or almost $420 in savings per member annually.3
Here’s a sample process related to payment policy:
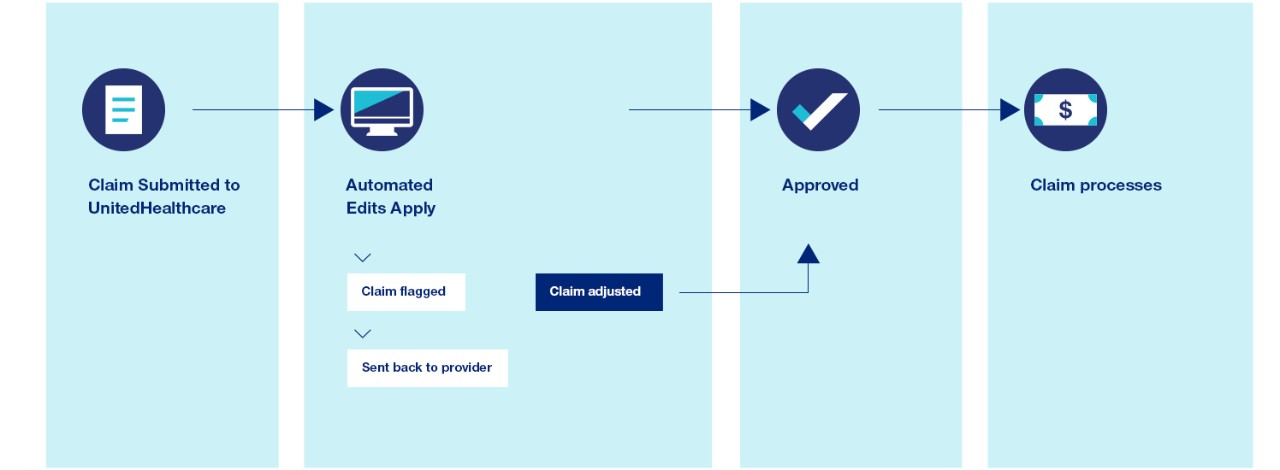
Accurate payments strengthen provider relationships
In addition to this focus on medical claims, working with providers is another key element in any successful payment integrity program. This includes UnitedHealthcare programs that place regional account managers on-site at hospitals across the country to provide immediate attention to recovering overpaid claims.
“We’re constantly providing feedback to help providers submit claims as accurately as possible because that prevents mispayments down the road,” Laubsted says. “If we identify an error and correct how that provider submits future claims, everyone benefits because we will no longer have to find and correct those errors. It’s a more efficient process for everyone.”
Leading the way in payment integrity solutions
UnitedHealthcare administers or supervises payment integrity solutions. Optum, a UnitedHealth Group company that executes many of UnitedHealthcare’s payment integrity solutions, was one of two payment integrity providers recognized as a “leader” by Everest Group, an independent third party. Everest measured providers on several criteria, including market impact, vision and capabilities.4
As an issue that affects the bottom line for employers and their employees, health care fraud demands serious and strategic solutions. To learn more about payment integrity solutions, reach out to your consultant, broker or UnitedHealthcare representative.