An untold cost-control story: The role of payment integrity- Image Transcript
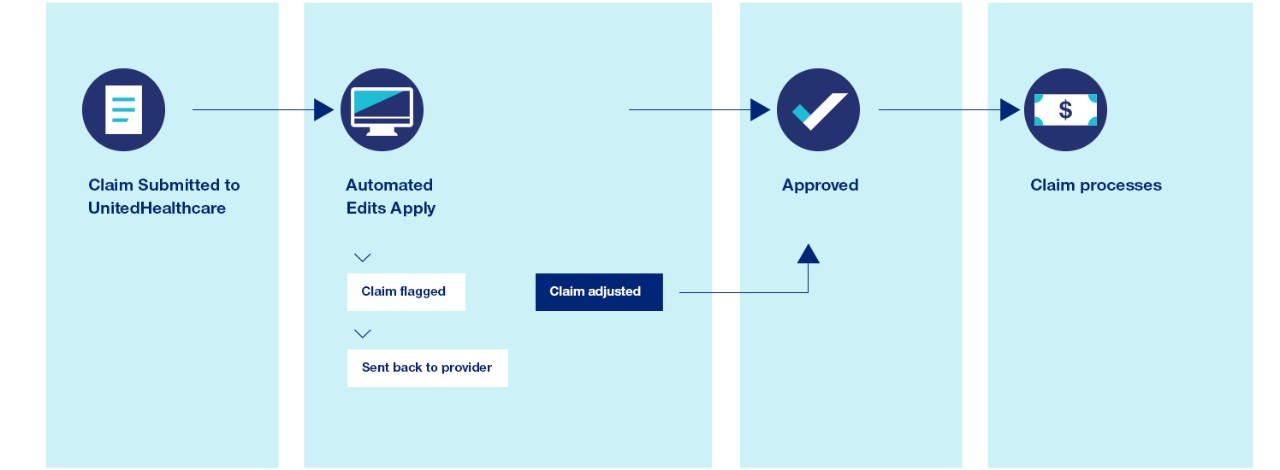
Claim Submitted to UnitedHealthcare.
Automated Edits Apply.
Claim is either flagged and sent back to provider or it’s adjusted and moves to approval. It’s then approved and the claim processes.